Postabortion Family Planning: A critical component of postabortion care
Background
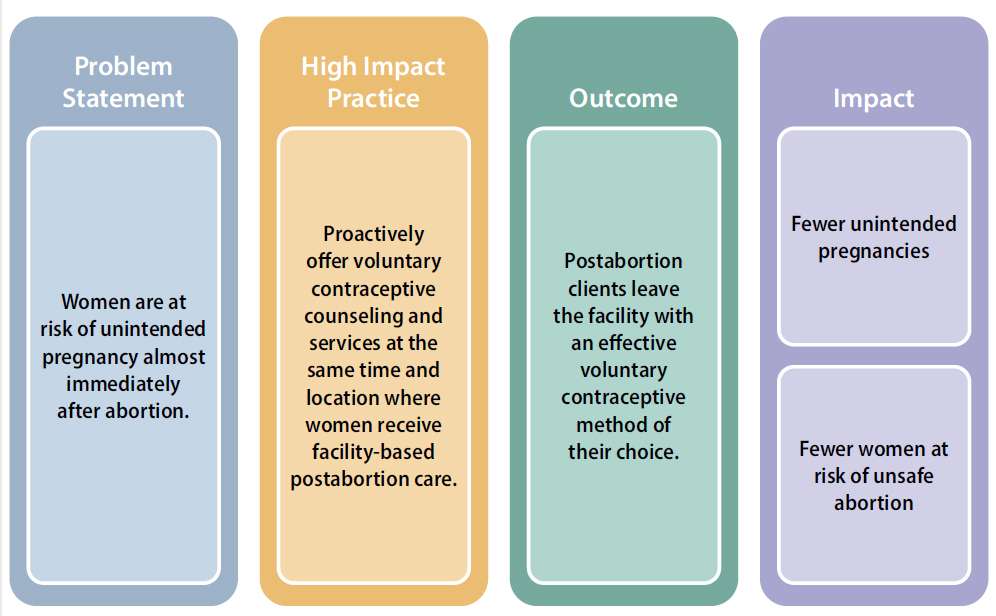
Postabortion care (PAC), which includes treatment for complications from miscarriage or induced abortion, is an opportune time to counsel and offer clients voluntary contraception. Even if a woman wants to become pregnant again soon, she should probably wait six months to reduce the chances of low birth weight, premature birth, and maternal anemia.*,[1] All PAC models include two essential services: (1) treatment of emergency complications, and (2) voluntary family planning counseling, including provision of contraception.3 Research studies and data from program implementation consistently show that when clients are counseled and offered contraception as part of postabortion care most women will opt to leave the facility with an effective family planning method (see Figure 1).4
Despite this evidence and decades of investments to improve PAC programs, health care systems continue to fall short. In Bangladesh, only 18% of all facilities providing PAC routinely offer contraceptive methods to clients.5 Similarly, only 6% of clients in Georgia, 17% in Tanzania, and 26% in Pakistan receive their contraceptive method of choice as part of PAC.6-8 Furthermore, studies in Kenya and Nepal show that even when services are in place, method choice may be limited.9,10 In Kenya, 9 of 10 postabortion clients left the facility with a method, but the vast majority left with male condoms due to limited contraceptive choice.9 The study also found significant gaps in information provided to clients, such as how to use the method correctly and follow-up information. In Brazil, only one-third of postabortion clients reported being counseled on contraception and less than 1 in 10 left the facility with a contraceptive method.11
Postabortion family planning is one of several High Impact Practices in Family Planning (HIPs) identified by a technical advisory group of international experts. When scaled up and institutionalized, HIPs will maximize investments in a comprehensive family planning strategy.12 For more information about other HIPs, see http://www.fphighimpactpractices.org/overview.
* A systematic review and meta-analysis suggests that an interval of less than six months following miscarriage is not associated with adverse outcomes.2 The meta-analysis was mainly of studies from developed countries.
It is recommended that programs implementing postabortion family planning include the following indicators:
- Percentage of postabortion clients who were counseled on family planning (disaggregated by age group, <20 years vs. ≥20 years)
- Percentage of postabortion clients who leave the facility with a modern contraceptive (disaggregated by type of method and age group, <20 years vs. ≥20 years)
What challenges can postabortion family planning help countries address?
Postabortion family planning can reach many women and girls in need of contraceptive counseling and services. Induced and spontaneous abortions (miscarriages) are common. Together, they account for an estimated one-quarter of all pregnancies worldwide.13 Globally, the number of induced abortions is on the rise, increasing from 50.2 million in 1990–1994 to 55.9 million in 2010–2014. Nearly half of these are considered unsafe, with the overwhelming number being in developing countries.14,15 Moreover, while induced abortions fell by 44% in developed regions (from 11.8 million to 6.6 million), they increased by 28% in developing regions (from 38.4 million to 49.3 million).15
Postabortion family planning can help clients achieve their reproductive intentions and is likely to provide cost savings for women, families, and the health system. Individuals and health systems alike bear significant costs for treating complications from unsafe abortions. In many African countries, a high proportion (15%–30%) of hospital gynecological admissions are due to complications of unsafe induced abortion.16 Treatment for abortion-related complications can consume nearly half of obstetrics and gynecology budgets.16 Costs could be reduced by investing in improving access to high-quality family planning services and increasing fertility awareness. Subsequent abortions are common17,18 and are an indication that the health system failed to facilitate access to effective contraceptives and information during the woman’s first encounter with PAC. One multi-country review found that, on average, nearly 20% of postabortion clients reported having had a previous induced abortion.19 Furthermore, more than half of postabortion clients expressed an interest in using contraception, yet only about one-quarter (27%) left the facility with a contraceptive method. Providing voluntary contraception to women who wish to delay or limit childbearing would cost just a fraction of the average expenditure on PAC: one year of modern contraceptive services and supplies costs, on average, 3%–12% of the cost of treating a PAC patient.20
Many postabortion clients and health workers do not know that postabortion clients are at risk of pregnancy almost immediately after abortion. Fertility can return within two weeks after a first-trimester abortion or miscarriage, within 4 weeks after a second-trimester abortion or miscarriage,1 and, on average, within three weeks following medical abortion with mifepristone or misoprostol.21 However, one cross-sectional study showed that nearly two-thirds of women who received PAC did not know when fertility returns after abortion, and this same group was not intending to use contraception despite three-quarters wanting to postpone childbearing.22 Women who leave a facility without a clear understanding of their pregnancy risk are almost three times more likely to have another abortion than women with accurate knowledge.23 Timely family planning counseling and services can help women prevent a subsequent unplanned pregnancy and possible abortion.
Unsafe abortion is a major contributor to maternal morbidity and mortality in developing countries, and postabortion family planning can reduce subsequent abortions. Globally, an estimated 25 million unsafe abortions occur each year,24 and between 4.7% and 13.2% of maternal deaths each year can be attributed to unsafe abortion.25 Around 7 million women are admitted to hospitals every year in developing countries as a result of unsafe abortion.15 The annual cost of treating major complications from unsafe abortion is estimated at US$553 million.20 Unsafe abortion is the fifth leading direct cause of pregnancy-related maternal mortality.25 Preventing unintended pregnancy, including among PAC clients, is fundamental to reducing the consequences of unsafe abortion.
What is the evidence that postabortion family planning is high impact?
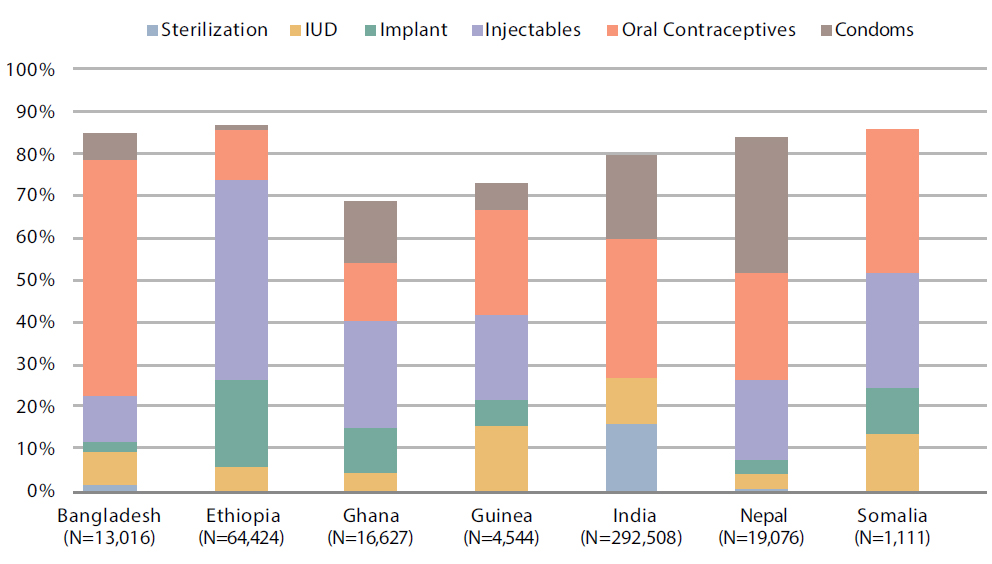
Across a wide variety of settings, data consistently show that acceptance of contraception is high when women are offered counseling and services as part of PAC. A review of evidence from the last 20 years concluded, “Postabortion family planning uptake generally increases rapidly—and unintended pregnancies and repeat abortions can decline as a result—when a range of free contraceptives, including long-acting methods, are offered at the point of treatment …”4 These findings are consistent with earlier systematic reviews.26 Rates of contraceptive uptake in small-scale intervention studies range between 25% and 98%.27,28 Figure 2 provides illustrative examples of voluntary contraceptive uptake achieved in large-scale routine service delivery programs when high-quality postabortion family planning services were in place.
Postabortion family planning reduces unplanned pregnancy and subsequent abortions. Studies show that providing voluntary family planning services as part of PAC can increase contraceptive use and reduce subsequent abortions. In Zimbabwe, postabortion clients who were referred to a nearby maternal and child health facility and charged a nominal fee for contraception were more than three times as likely to experience an unplanned pregnancy in the 12 months following an abortion as postabortion clients who were offered on-site, ward-based family planning services and methods for free.33 Similarly, in Georgia multiple abortions were significantly more common among women who did not receive postabortion contraception at the site of PAC compared with those who did.6
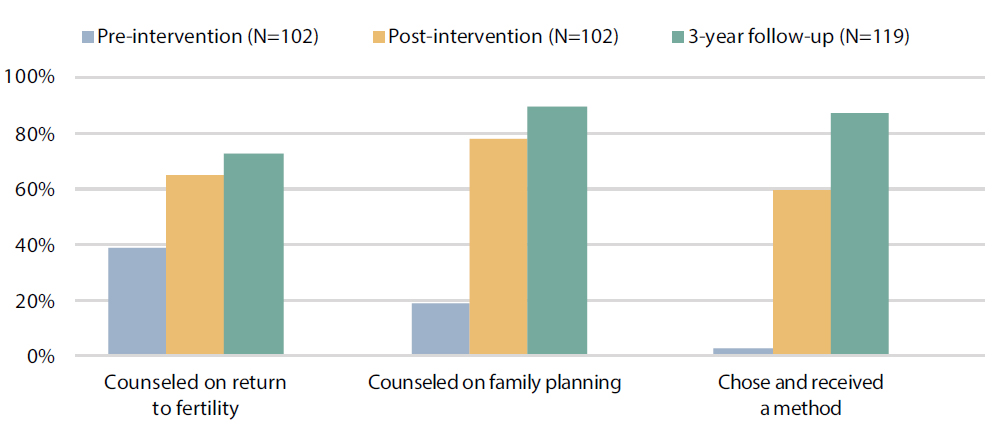
Postabortion family planning is scalable and sustainable, and program effectiveness can increase over time. The programs included in Figure 2 represent large-scale implementation in a diverse range of settings. Figure 3 shows data from Peru, where institutions have strengthened the family planning component of PAC and sustained or improved on these gains well after technical assistance ended.34 Specifically, three years after technical assistance ended, over 80% of postabortion clients received a method prior to leaving the facility compared with just under 60% during the technical assistance period. Similar findings have been shown in Turkey.28
How to do it: Tips from implementation experience
Offering information and services to women at the same place and time they receive facility-based PAC is key to implementing effective PAC services. Additionally implementers should consider the following elements in their programs.
Address stigma and social and community barriers. Abortion is often stigmatized, particularly in settings where abortion is legally restricted. Seeking care to address complications of abortion or to choose a contraceptive method can be particularly difficult for individuals in these settings or among individuals whose autonomy is limited because choosing to use a method implies her abortion was induced.4 Offering family planning counseling and voluntary contraception to all postabortion clients—both those seeking treatment for miscarriage and those seeking treatment for induced abortion—helps reduce that potential stigma.
- Engage communities and community health workers. In Kenya, training community health workers to raise awareness and change community attitudes about PAC and to counsel women about family planning increased both the number of women using PAC services and the number using contraception. According to program implementers, the vast majority of PAC clients were referred by community health workers. A key approach is to engage communities in dialogue to define the need for PAC services, design PAC services that fit within the community culture, and develop local ownership for ensuring equitable access to and quality of PAC.35-37
- Engage support networks. Many women want their partner, husband, or other support person present for PAC counseling.4 After discussing the client’s preferences, including loved ones in counseling and clinical instruction has been shown to improve adherence to care instruction.38
Offer PAC at primary care facilities and allow nurses and midwives to provide care in order to expand access and reduce costs. Several countries, such as Ghana, Kenya, Mozambique, Nepal, Senegal, Tanzania, and Uganda, have demonstrated that trained, competent nurses and midwives can provide PAC services safely.39-44 Task-sharing policies that expand the range of health care workers who can provide PAC, including family planning, may result in cost savings for the health system by reducing the work load at tertiary care facilities.45,46 Several international health professional associations have endorsed this approach.3 Task sharing may also result in savings for clients by making services more convenient and easier to access. Midwives and nurses are more widely accessible than physicians to women in remote or underserved areas. In addition, some studies have shown that establishing family planning as part of PAC services is easier in places where midwives are responsible for all reproductive health services.39
Invest in quality. In Bangladesh, clients who rated the postabortion services they received as medium- or high-quality were more likely to report using contraception three months later than clients who rated their services as low-quality.47 Some of the elements of quality care include the following:
- Offer a wide range of contraceptive methods. Offering a wide range of methods, including long-acting methods, is likely to increase voluntary family planning uptake.4 In Honduras, after introducing a wider range of contraceptive methods, the percentage of PAC clients leaving with a method increased from 13% to 54% after 20 months.48 In Cambodia, the predicted probability of a client leaving with a contraceptive method was significantly higher in facilities offering more than four methods than in facilities offering one to three methods (42% versus 18%, respectively).49
- Encourage and support providers to treat all clients respectfully. Such support often includes, but is not limited to, provider training and values clarification to address provider bias. Training should be reinforced through supportive supervision, job descriptions, operational guidelines and policies, and other types of institutional support.
- Link clients to resources for ongoing support. After initiating a contraceptive method, provide clients with information on where to access ongoing support and resupply, if necessary. Offer clients written instructions about how to use their preferred method for future reference. Digital technologies, hotlines, and community health workers may provide additional means to support clients. While offering follow-up support, health workers should be sensitive to client preferences and respectful of client privacy. Providing family planning counseling at follow-up visits is also an important factor in reducing subsequent abortions.33,50

Address the needs of PAC clients facing gender-based violence. Multiple studies highlight the relationship between gender-based violence and the increased risk of spontaneous abortion and/or increased likelihood to seek induced abortion.51-56 Addressing these particular needs within PAC services requires training health care providers on how to identify survivors of intimate partner violence and sexual violence and respond to their needs, in addition to providing the necessary clinical care.32,57
Make contraception free or bundle it with the cost of postabortion treatment. In Burkina Faso, the cost of postabortion contraception is a significant barrier for many PAC clients.58 For adolescents and other vulnerable women, costs contribute to delays in seeking PAC as well as in accessing family planning before discharge from the facility. In Senegal, management of client payments often leads to cumbersome processes, which serve as a barrier to access.59 In Tanzania, where PAC and family planning services are supposed to be free, the average total out-of-pocket cost for PAC clients was more than US$20 (including transportation and treatment of complications, but with no charge for contraception).60 In Russia, the financial cost of an abortion is substantially lower than the cost of using pills or condoms for a year.50 Free contraception, waivers for poor and vulnerable clients, and streamlined payment systems are likely to enhance equitable access to contraception for PAC clients.
Ensure equitable access to postabortion contraception, regardless of:
- Client’s age. In Kenya postabortion youth clients between the ages of 15 and 24 were less likely to receive a contraceptive method compared with adult clients (35% versus 48%, respectively), and 49% of youth reported not using contraception due to concerns of infertility, side effects, or lack of knowledge, compared with 22% of adults.61 Specialized training on youth-friendly PAC was associated with a sustained greater voluntary uptake of contraception among young women in Ethiopia when compared with standard training.62 Several countries including Angola, Ethiopia, Ghana, Kenya, Mozambique, Nigeria, Tanzania, and Uganda have assessed the quality of PAC for younger clients, and assessment tools are available.63
- Local contexts. In humanitarian settings, women and girls may be at increased risk of unintended pregnancy and unsafe abortion. Furthermore, they may not be able to continue with their contraceptive method as it was lost during displacement. Women, girls, and couples may not wish to become pregnant during a crisis situation and prefer to wait until security returns, livelihoods are assured, and their situation stabilizes.64 Research has documented that approximately one in five women in complex humanitarian settings experienced sexual violence, which is likely an underestimate.65 In Puntland, Somalia, an area of chronic conflict, an NGO implemented a package of interventions including competency-based training of providers, community engagement including with religious leaders, regular use of data for decision making, and medical supply chain strengthening. 98% of PAC clients were counseled on contraception, 88% of whom accepted a contraceptive method before leaving the facility, demonstrating that comprehensive PAC services can be successfully implemented in politically unstable and culturally conservative settings.31
- The type of evacuation procedure received. All contraceptives, with a few exceptions, can be offered after surgical or medical evacuation for treating complications (see Box 1). Most can be initiated on the day of treatment. However, postabortion family planning may be more or less frequently offered to women based on which evacuation procedure they received.4,66 Family planning services should be offered to all postabortion clients on-site irrespective of evacuation procedure as an integral part of PAC.67
Can start immediately:
- Hormonal methods: implants, monthly injectables, injectables, combined oral contraceptive pills, progestin-only pills, progestin-only injectables, combined patch, emergency contraceptive pills.
- Barrier methods: male or female condoms.
- Intrauterine devices (IUDs): copper-bearing or levonorgestrel-releasing. These can be provided immediately after emergency treatment of complications if there is no infection—or when infection is ruled out and resolved, and any injury has healed. However, IUD insertion following medical treatment of emergency complications requires the patient to return for a follow-up visit.
- Diaphragms, cervical caps, and combined vaginal ring: can be offered once injury is ruled out or after any injury to the genital tract has healed.
- Permanent methods: tubal ligation or vasectomy (for her partner). Permanent methods can be offered after the client has had time to rest and recover from any sedation, and is not stressed or in pain. Counsel carefully and be sure to mention available reversible methods.
Delay use:
- Fertility awareness methods: Standard Days Method or TwoDay Method. It is recommended that women start these methods after their regular menstrual pattern returns.
Source: WHO (2018).1
Postabortion Care e-learning course (published May 2018) provides an overview of postabortion care including its definition, objectives, justification, programming best practices, indicators for monitoring and evaluation, and strong evidence base, including evidence-based approaches to strengthen postabortion family planning. Available in English from https://www.globalhealthlearning.org/course/postabortion-care-pac.
Postabortion Care resource site is a one-stop source for basic instruments to assist policy makers, program managers, clinical staff, and donors in program design, implementation, and evaluation. Available in English and French from http://www.postabortioncare.org/.
Family Planning: A Global Handbook for Providers (2018 edition) includes a section on family planning in postabortion care. Users can download printable files or order a copy of the handbook at http://www.fphandbook.org/order-form.
For more information about High Impact Practices in Family Planning (HIP), please contact the HIP team.
Search Strategy
To compile the list of postabortion family planning (PAFP) documents meeting inclusion criteria, a literature search was conducted using bibliographic databases and hand searching of online websites for journal and grey literature. The period of review focused on documents published after the previous HIP brief on PAFP was developed in 2012 through April 2018.
For more information, download the Methods for literature search, information sources, abstraction and synthesis document.
References
- World Health Organization, Department of Reproductive Health and Research (WHO/RHR); Johns Hopkins Bloomberg School of Public Health/Center for Communication Programs (CCP), Knowledge for Health Project. Family Planning: A Global Handbook for Providers. 2018 update. Baltimore and Geneva: CCP and WHO; 2018. https://www.fphandbook.org/. Accessed February 27, 2019.
- Kangatharan C, Labram S, Bhattacharya S. Interpregnancy interval following miscarriage and adverse pregnancy outcomes: systematic review and meta-analysis. Hum Reprod Update. 2017;23(2):221-231. https://doi.org/10.1093/humupd/dmw043
- International Federation of Gynecology and Obstetrics (FIGO); International Confederation of Midwives (ICM); International Council of Nurses (ICN); United States Agency for International Development (USAID); White Ribbon Alliance (WRA); Department for International Development (DFID); Bill & Melinda Gates Foundation. Post abortion family planning: A key component of post abortion care. Washington, DC: 2013. https://www.figo.org/sites/default/files/uploads/project-publications/PAC-FP-Joint-Statement-November2013-final_printquality.pdf. Accessed February 27, 2019.
- Huber D, Curtis C, Irani L, Pappa S, Arrington L. Postabortion care: 20 years of strong evidence on emergency treatment, family planning, and other programming components. Glob Health Sci Pract. 2016;4(3):481-494. https://doi.org/10.9745/GHSP-D-16-00052
- Hossain A, Maddow-Zimet I, Ingerick M, Bhuiyan HU, Vlassoff M, Singh S. Access to and quality of menstrual regulation and postabortion care in Bangladesh: evidence from a survey of health facilities, 2014. New York: Guttmacher Institute; 2017. https://www.guttmacher.org/sites/default/files/report_pdf/menstrualregulationpostabortion-care-bangladesh_0.pdf. Accessed February 27, 2019.
- Pestvenidze E, Berdzuli N, Lomia N, Gagua T, Umikashvili L, Stray-Pedersen B. Repeat induced abortions in Georgia, characteristics of women with multiple pregnancy terminations: secondary analysis of the Reproductive Health Survey 2010. Eur J Obstet Gynecol Reprod Biol. 2016;205:85-90. https://doi.org/10.1016/j.ejogrb.2016.08.020
- EngenderHealth. Post Abortion Care-Family Planning Annual Report for the Period October 1, 2016 – September 30, 2017. New York: EngenderHealth; 2017.
- Zaidi S, Yasmin H, Hassan L, Khakwani M, Sami S, Abbas T. Replacement of dilation and curettage/evacuation by manual vacuum aspiration and medical abortion, and the introduction of postabortion contraception in Pakistan. Int J Gynaecol Obstet. 2014;126(suppl 1):S40-S44. https://doi.org/10.1016/j.ijgo.2014.03.016 Postabortion Family Planning Postabortion Family Planning: A critical component of postabortion care Service Delivery HIP Proven Practice 2 April 2019
- Mutua MM, Achia TNO, Maina BW, Izugbara CO. A cross-sectional analysis of Kenyan postabortion care services using a nationally representative sample. Int J Gynaecol Obstet. 2017;138(3):276-282. https://doi.org/10.1002/ijgo.12239
- Rocca CH, Puri M, Harper CC, Blum M, Dulal B, Henderson JT. Postabortion contraception a decade after legalization of abortion in Nepal. Int J Gynaecol Obstet. 2014;126(2):170-174. https://doi.org/10.1016/j.ijgo.2014.02.020
- Borges AL, Monteiro RL, Hoga LA, Fujimori E, Chofakian CB, dos Santos OA. Post-abortion contraception: care and practices. Rev Lat Am Enfermagem. 2014;22(2):293-300. https://dx.doi.org/10.1590%2F0104-1169.3240.2415
- High Impact Practices in Family Planning (HIP). Family planning high impact practices list. Washington, DC: USAID; 2018. https://www.fphighimpactpractices.org/high-impact-practices-in-family-planning-list/. Accessed February 27, 2019.
- Sedgh G, Bearak J, Singh S, et al. Abortion incidence between 1990 and 2014: global, regional, and subregional levels and trends. Lancet. 2016; 388(10041):258-267. https://doi.org/10.1016/S0140-6736(16)30380-4
- Sedgh G, Singh S, Shah IH, Ahman E, Henshaw S, Bankole A. Induced abortion: incidence and trends worldwide from 1995 to 2008. Lancet. 2012;379(9816):625-632. https://doi.org/10.1016/S0140-6736(11)61786-8
- Singh S, Remez L, Sedgh G, Kwok L, Onda T. Abortion worldwide 2017: uneven progress and unequal access. New York: Guttmacher Institute; 2018. https://www.guttmacher.org/sites/default/files/report_pdf/abortionworldwide2017.pdf. Accessed February 27, 2019.
- Lule E, Singh S, Chowdhury SA. Fertility regulation behaviors and their costs: contraception and unintended pregnancies in Africa and Eastern Europe and Central Asia. Washington, DC: World Bank; 2007. http://siteresources.worldbank.org/HEALTHNUTRITIONANDPOPULATION/Resources/281627-1095698140167/FertilityRegulationsFinal.pdf. Accessed February 27, 2019.
- Jones RK, Singh S, Finer LB, Frohwirth LF. Repeat abortion in the United States. New York: Guttmacher Institute; 2006. Occasional Report 29. http://www.guttmacher.org/pubs/2006/11/21/or29.pdf. Accessed February 27, 2019.
- Peipert JF, MaddenT, Allsworth JE, Secura, GM. Preventing unintended pregnancies by providing no-cost contraception. Obstet Gynecol. 2012;120(6):1291-1297. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4000282/
- Kidder E, Sonneveldt E, Hardee K. Who receives PAC services? Evidence from 14 countries. Washington, DC: The Futures Group; 2004.
- Vlassoff M, Singh S, Onda T. The cost of postabortion care in developing countries: a comparative analysis of four studies. Health Policy Plan. 2016; 31(8):1020-1030. http://doi.org/10.1093/heapol/czw032
- Schreiber CA, Sober S, Ratcliffe S, Creinin MD. Ovulation resumption after medical abortion with mifepristone and misoprostol. Contraception. 2011;84(3):230-233. https://doi.org/10.1016/j.contraception.2011.01.013
- Mahmoud GA, Byomy SS. Fertility awareness and family planning use among post abortion women in Egypt. Life Sci J. 2013;10(1):143-150. https://www.dx.doi.org/10.7537/marslsj100113.21 April 2019 3
- David PH, Reichenbach L, Savelieva I, Vartapetova N, Potemkina R. Women’s reproductive health needs in Russia: what can we learn from an intervention to improve post-abortion care? Health Policy Plan. 2007;22(2):83-94. https://doi.org/10.1093/heapol/czm003
- Ganatra B, Gerdts C, Rossier C, et al. Global, regional, and subregional classification of abortions by safety, 2010-14: estimates from a Bayesian hierarchical model. Lancet. 2017;390(10110):2372-2381. https://doi.org/10.1016/S0140-6736(17)31794-4
- Say L, Chou D, Gemmill A, et al. Global causes of maternal death: a WHO systematic analysis. Lancet Glob Health. 2014;2(6):e323-33. http://dx.doi.org/10.1016/S2214-109X(14)70227-X
- Tripney J, Kwan I, Bird, KS. Postabortion family planning counseling and services for women in low income countries: a systematic review. Contraception. 2013;87(1):17-25. https://doi.org/10.1016/j.contraception.2012.07.014
- Centre de Formation et de Recherche en Sante de la Reproduction (CEFOREP). Introduction des soins obstetricaux d’urgence et de la planification familiale pour les patients presentant des complications liees a un avortement incomplete. Dakar: CEFOREP; 1998.
- Senlet P, Cagatay L, Ergin J, Mathis J. Bridging the gap: integrating family planning with abortion services in Turkey. Int Fam Plan Perspect. 2001;27(2):90-95. https://www.guttmacher.org/sites/default/files/article_files/2709001.pdf. Accessed March 15, 2019.
- Benson J, Andersen K, Brahmi D, et al. What contraception do women use after abortion? An analysis of 319,385 cases from eight countries. Glob Public Health. 2018;13(1):35-50. https://doi.org/10.1080/17441692.2016.1174280
- Banerjee SK, Gulati S, Andersen KL, Acre V, Warvadekar J, Navin D. Associations between abortion services and acceptance of postabortion contraception in six Indian states. Stud Fam Plann. 2015;46(4):387-403. https://doi.org/10.1111/j.1728-4465.2015.00039.x
- Chukwumalu K, Gallagher MC, Baunach S, Cannon A. Uptake of postabortion care services and acceptance of postabortion contraception in Puntland, Somalia. Reprod Health Matters. 2017;25(51):48-57. https://doi.org/10.1080/09688080.2017.1402670
- Pfitzer A, Hyjazi Y, Arnold B, et al. Inclusion of long-acting reversible contraceptives as an option for postabortion care clients in Guinea: results of an observational study. Glob Health Sci Pract. 2019;7(suppl 2). In press
- Johnson BR, Ndhlovu S, Farr SL, Chipato T. Reducing unplanned pregnancy and abortion in Zimbabwe through postabortion contraception. Stud Fam Plann. 2002;33(2):195-202. https://doi.org/10.1111/j.1728-4465.2002.00195.x
- Benson J, Huapaya V. Sustainability of postabortion care in Peru. New York: Population Council; 2002. 45 p. https://www.popline.org/node/235774. Accessed February 27, 2019.
- Ottolenghi E, Riveros P, Blanding S. Assessment of the Bolivia Postabortion Care Community Mobilization Program. ACQUIRE Project; 2008. http://www.acquireproject.org/archive/files/5.0_community_engagement_
marketing_and_communications/5.2_resources/5.2.2_studies/cPAC_report_revised_final.pdf. Accessed on March 18, 2019. 4 April 2019 - Undie CC, Obare F, RamaRao S. Replication of the Community Mobilization for Postabortion Care (COMMPAC) model in Naivasha District, Rift Valley Province, Kenya: evaluation report. The RESPOND Project Study Series: Contributions to Global Knowledge Report No. 9. New York: EngenderHealth; 2012. http://www.respond-project.org/pages/files/6_pubs/research-reports/Study9-COMMPAC-Final-Evaluation-December2012-Final-forweb.pdf. Accessed February 27, 2019.
- Wickstrom J, Russell N, Escandon I. Engaging communities as partners in postabortion care: a desk review of the Community Postabortion Care Project in Nakuru, Kenya. ACQUIRE Evaluation and Research Studies No. 11. New York: The ACQUIRE Project/Engender Health; 2008. http://www.acquireproject.org/archive/files/11.0_research_studies/er_study_11.pdf. Accessed February 27, 2019.
- Abdel-Tawab N, Huntington D, Hassan EO, Youssef H, Nawar L. Effects of husband involvement in postabortion patients’ recovery and use of contraception in Egypt. In: Huntington D, Piet-Pelon NJ, editors. Postabortion Care: Lessons from Operations Research. New York: Population Council; 1999. pp. 16-37.
- Kiggundu C. Decentralizing integrated postabortion care in Uganda: a pilot training and support initiative for improving the quality and availability of integrated RH service. Kampala, Uganda: Ministry of Health, PRIME, Ipas, and DISH; 1999.
- Population Council. Improving the counseling and medical care of post abortion patients in Egypt: final report. Cairo, Eygpt: Population Council; 1995. p. 215.
- Billings D, Victor A, Baird T, Taylor J, Ababio K, Ntow S. Midwives and comprehensive postabortion care in Ghana. In: Huntington D, Piet-Pelon N, eds. Postabortion Care: Lessons from Operations Research. New York: Population Council; 1999. pp. 141-158.
- Extending Service Delivery (ESD). A description of the private nurse midwives networks (clusters) in Kenya: a best practice model. Best Practices Series Report No. 2. Washington, DC: Pathfinder International, Extending Service Delivery Project; 2007.
- Basnet I, Clapham S, Shaka G, McCall M. Evolution of the postabortion care program in Nepal: the contribution of a national safe motherhood project. Int J Gynaecol Obstet. 2004;86(1):98-108. https://doi.org/10.1016/j.ijgo.2004.03.014
- Wanjiru M, Askew I, Munguti N, RamaRao S, Homan R. Assessing the feasibility, acceptability and cost of introducing postabortion care in health centres and dispensaries in rural Tanzania. Washington, DC: Population Council; 2007. http://pdf.usaid.gov/pdf_docs/PNADJ505.pdf. Accessed on February 27, 2019.
- Johnston HB, Gallo MF, Benson J. Reducing the costs to health systems of unsafe abortion: a comparison of four strategies. J Fam Plann Reprod Health Care. 2007;33(4):250–257. http://dx.doi.org/10.1783/147118907782101751
- Brambila C et al. Estimating costs of postabortion services at Dr. Aurelio Valdivieso General Hospital, Oaxaca, Mexico. In: Huntington D, Piet-Pelon N, ed. Postabortion Care: Lessons from Operations Research. New York: Population Council; 1999. pp. 108–124.
- Sultana F, Nahar Q, Marions L, Oliveras E. Effect of post-menstrual regulation family planning service quality on subsequent contraceptive use in Bangladesh. Int J Gynaecol Obstet. 2013;123(suppl 1):e38-e42. http://dx.doi.org/10.1016/j.ijgo.2013.07.007
April 2019 5 - Medina R, Vernon R, Mendoza I, Aguilar C. Expansion of postpartum/postabortion contraception in Honduras. New York: Population Council; 2001. http://pdf.usaid.gov/pdf_docs/Pnacm374.pdf. Accessed on February 27, 2019.
- McDougall J, Fetters T, Clark KA, Rathavy T. Determinants of contraceptive acceptance among Cambodian abortion patients. Stud Fam Plann. 2009;40(2): 123-32. http://dx.doi.org/10.1111/j.1728-4465.2009.00195.x
- Savelieva I, Pile JM, Sacci I, Loganathan R. Postabortion family planning operations research study in Perm, Russia. New York: Population Council; 2003. http://pdf.usaid.gov/pdf_docs/pnacu602.pdf. Accessed on February 27, 2019.
- Gessessew A. Abortion and unwanted pregnancy in Adigrat Zonal Hospital, Tigray, North Ethiopia. Afr J Reprod Health. 2010:14(3):183-188. http://www.bioline.org.br/pdf?rh10034. Accessed on March 15, 2019.
- Hakimi M, Hayati EN, Marlinawati VU, Winkvist A, Ellsberg MC. Silence for the sake of harmony: domestic violence and health in Central Java, Indonesia. Yogyakarta, Indonesia: Umea University; 2001. https://www.popline.org/node/571345. Accessed on February 27, 2019.
- Heise L, Ellsberg M, Gottemoelle M. Ending violence against women. Population Reports. Series L: Issues in World Health. Baltimore, MD: Johns Hopkins School of Public Health, Population Information Program; 1999. http://www.k4health.org/toolkits/info-publications/ending-violence-against-women. Accessed on February 27, 2019.
- Kaye DK, Mirembe FM, Bantebya G, Johansson A, Ekstrom AM. Domestic violence as risk factor for unwanted pregnancy and induced abortion in Mulago Hospital, Kampala, Uganda. Trop Med Int Health. 2006;11(1):90-101. https://doi.org/10.1111/j.1365-3156.2005.01531.x
- Keeling J, Birch L, Green P. Pregnancy counseling clinic: a questionnaire survey of intimate partner abuse. J Fam Plann Reprod Health Care. 2004;30(3):165-168. http://dx.doi.org/10.1783/1471189041261663
- Silverman JG, Gupta J, Decker MR, Kapur N, Raj A. Intimate partner violence and unwanted pregnancy, miscarriage, induced abortion, and stillbirth among a national sample of Bangladeshi women. BJOG. 2007;114(10):1246-1252. https://doi.org/10.1111/j.1471-0528.2007.01481.x
- World Health Organization (WHO). Responding to intimate partner violence and sexual violence against women: WHO clinical and policy guidelines. Geneva: WHO; 2013. https://www.who.int/reproductivehealth/publications/violence/9789241548595/en/. Accessed on February 27, 1029.
- Fikree FF, Mugore S, Forrester H. Strengthening postabortion family planning in Burkina Faso: pre-service and in-service training on postabortion care. Washington, DC: Pathfinder International, Evidence to Action for Strengthened Reproductive Health; 2014. https://www.e2aproject.org/wp-content/uploads/strengthening-pac-fpburkina.pdf. Accessed on February 27, 2019.
- Fikree FF, Mugore S, Forrester H. Strengthening postabortion family planning in Senegal: maintaining and enhancing postabortion care services. Washington, DC: Pathfinder International, Evidence to Action for Strengthened Reproductive Health; 2014. https://www.e2aproject.org/wp-content/uploads/strengthening-pacfp-senegal.pdf. Accessed on February 27, 2019. 6 April 2019
- EngenderHealth. Health system and patient cost for scaling up post abortion and post abortion care family planning services in Tanzania, 2018. New York: EngenderHealth; [2018].
- Evens E, Otieno-Masaba R, Eichleay M, et al. Post-abortion care services for youth and adult clients in Kenya: a comparison of services, client satisfaction and provider attitudes. J Biosoc Sci. 2014;46(1):1-15. https://doi.org/10.1017/S0021932013000230
- Alemayehu T, Biru D, Hendrickson C, Brahmi D, Fetters T. An evaluation of postabortion contraceptive uptake following a youth-friendly services intervention in Ethiopia. Chapel Hill, NC: Ipas; 2016. https://endabortionstigma.org/~/media/Files/PubsManual/PMDETHE16.ashxutm_source=resource&utm_medium=meta&utm_campaign=PMDETHE16. Accessed on February 27, 2019.
- Hainsworth G, Boyce C, Israel E. Assessment of youth-friendly postabortion care services: a global tool for assessing and improving postabortion care for youth. Watertown, MA: Pathfinder International; 2008. http://www2. pathfinder.org/site/DocServer/YFPAC_assessment_tool.pdf?docID=13121. Accessed on February 27, 2019.
- Interagency Working Group on Reproductive Health in Crisis (IAWG). Inter-Agency Field Manual on Reproductive Health in Humanitarian Settings. IAWG; 2018. http://iawg.net/iafm/. Accessed March 15, 2019.
- Vu A, Adam A, Wirtz A, et al. The prevalence of sexual violence among female refugees in complex humanitarian emergencies: a systematic review and meta-analysis. PLoS Curr. 2014;6:pii:ecurrents.dis.835f10778fd80ae031aac12d3b533ca7. https://doi.org/10.1371/currents.dis.835f10778fd80ae031aac12d3b533ca7
- Nielsen KK, Lusiola G, Kananma J, Bantamby J, Kikumbih N, Rasch V. Expanding comprehensive postabortion care to primary health facilities in Geita District, Tanzania. Afr J Reprod Health. 2009;13(2):129-38. http://www.bioline.org.br/pdf?rh09029. Accessed March 15, 2019.
- Rasch V, Massawe S, Yambesi F, Bergstrom S. Acceptance of contraceptives among women who had an unsafe abortion in Dar es Salaam. Trop Med Int Health. 2004;9(3):399-405. https://doi.org/10.1111/j.1365-3156.2004.01197.x
View the previous version of this HIP published in November 2012.
Suggested Citation
High Impact Practices in Family Planning (HIP). Postabortion family planning: a critical component of postabortion care. Washington, DC: USAID; 2019 Mar. Available from: https://www.fphighimpactpractices.org/briefs/postabortion-family-planning/
Acknowledgements
This brief was written by Erin Mielke, Douglas Huber, Carolyn Curtis, and Shawn Malarcher. It was updated from a previous draft authored by Julie Solo and Shawn Malarcher. Critical review and helpful comments were provided by Bethany Arnold, Michal Avni, Hashina Begum, Neelam Bhardwaj, Neeta Bhatnagar, Venkatraman Chandra-Mouli, Elaine Charurat, Arzum Ciloglu, Claudia Conlon, Sweta Das, Isha Datta, Rubee Dev, Erin Files Dumas, Christine Galavotti, Alison Gatto, Laura Ghiron, Kate Gilles, Roy Jacobstein, Antonella Francheska Lavelanet, Grace Lusiola, Sylvia Lynch, Cat McKaig, Alice Payne Merritt, Janet Meyers, Tembi Mugore, Poonam Muttreja, Jean Jose Nzau, Kim Ocheltree, Amelia Ngozi Odod, Japheth Ominde, Anne Pfitzer, May Post, Eric Ramirez, Laura Raney, Ruth Simmons, Sanghamitra Singh, Anand Sinha, Sara Stratton, Nandita Thatte, Caitlin Thistle, and Erick Yegon.
This HIP brief is endorsed by:
Bill & Melinda Gates Foundation, CARE, Chemonics International, Engender Health, FHI 360, FP2020, Georgetown University/Institute for Reproductive Health, International Planned Parenthood Federation, IntraHealth International, Jhpiego, John Snow, Inc., Johns Hopkins Center for Communication Programs, Palladium, PATH, Pathfinder International, Plan International USA, Population Council, Population Reference Bureau, Population Services International, Promundo US, Public Health Institute, Save the Children, U.S. Agency for International Development*, United Nations Population Fund, and University Research Co., LLC.
* USAID supports the treatment of injuries or illnesses caused by legal or illegal abortions and counseling on and provision of voluntary family planning options (Post-Abortion Care or PAC).
The World Health Organization/Department of Reproductive Health and Research has contributed to the development of the technical content of HIP briefs, which are viewed as summaries of evidence and field experience. It is intended that these briefs be used in conjunction with WHO Family Planning Tools and Guidelines: http://www.who.int/topics/family_planning/en/.
Provide Comments
To provide comments on this brief, please fill out the form on the Community Feedback page.