Social Accountability to improve family planning information and services
What is the high-impact practice in family planning?
Engage communities and health sector actors in a collaborative process to jointly identify problems, and to implement and monitor solutions to hold each other accountable for improvements in the quality and responsiveness of family planning services.
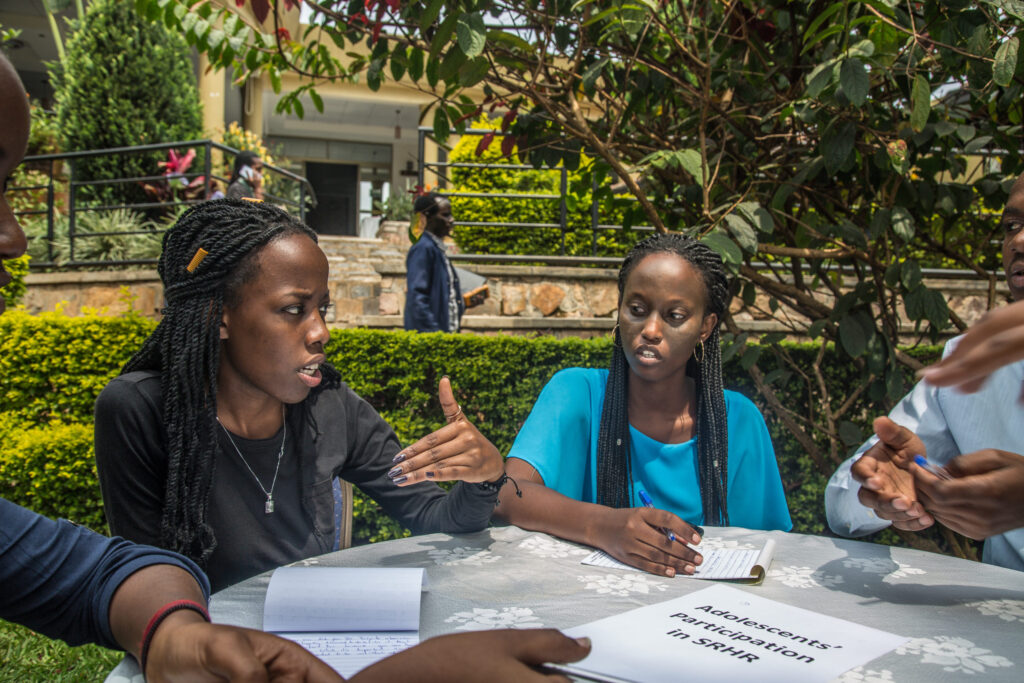
Health Development Initiative (HDI) was founded by Rwandan physicians with the goal of empowering individuals and communities to improve health and advance development. Credit: Images of Empowerment
Background
Collective efforts of individuals and communities (rights holders) to hold service providers, government officials, and other decision makers (duty bearers) to account for the quality, effectiveness, and equitable provision of services is referred to as “social accountability.”1–3 Grounded in human rights, social accountability is an evolving umbrella term that covers a range of approaches. Social accountability has taken place for many years and across multiple sectors,4–7 including more recently family planning.8
This brief focuses on social accountability approaches for family planning that are designed with the following criteria: 1) primarily operate at the subnational level, where the community and health facility intersect; 2) involve a high degree of community influence and control; 3) are largely collaborative in nature rather than confrontational; 4) facilitate community voice and bolster service provider/power holder responsiveness; and 5) are structured, facilitated, and transparent processes that create safe and inclusive space for effective dialogue and negotiation. A number of generic and branded tools have been developed to facilitate social accountability processes, including Community Score Card (CSC), Citizen Voice and Action (CVA), public hearings, and social audits (see Appendix for further descriptions of these approaches). This brief recognizes that despite the design of the approach, social accountability can sometimes result in confrontation between different actors given local power dynamics. Approaches should be facilitated to mitigate this, with tips provided in the “How to do it” section below.*
Social accountability to improve family planning information and services is one of several “high-impact practices in family planning” (HIPs) identified by the HIPs partnership and vetted by the HIPs Technical Advisory Group. For more information about HIPs, see https://fphighimpactpractices.org/overview/.
*Other accountability approaches, not covered in this brief, include tracking government and donor financial commitments, tracking specific elements of program implementation (e.g., commodity security, coverage indicators), legal accountability, and “pressure” campaigns by advocates and activists. These approaches may be suited to particular contexts or issues, and may at times be complementary to those described in this brief.3,9–12
Box 1. Social Accountability for Family Planning: The Process
This social accountability approach often starts with a non-governmental organization or local civil society organization initiating conversations with key health system stakeholders, during which the benefits of increasing dialogue between the community and health workers is shared and their support and co-ownership garnered. Next, a series of facilitated discussions with the community members, including key groups (e.g., women, youth, marginalized), are convened to solicit their concerns, discuss barriers to service use, and prioritize areas of most concern. A similar series of facilitated discussions is held with health providers to give them the opportunity to voice their concerns openly, and to prioritize the biggest problems from their perspective. Once all stakeholders have had a chance to be fully heard, an interface meeting can be held where each side shares challenges and concerns, and together prioritize the issues to tackle and discuss how these issues could be addressed. Solutions are generated and both sides commit to implementation. At regular intervals the community and health providers come back together to jointly review progress in an ongoing accountability process.
Theory of Change

What challenges can social accountability help countries address?
Services not aligned with community needs and preferences can impede service use. Negative attitudes of providers, and their own resource and technical constraints, can get in the way of providing high-quality services responsive to community needs. Social accountability can fundamentally change how communities and health system actors approach and address the challenges they face. When structured appropriately, these mechanisms can mitigate distrust and fear amongst stakeholders and evolve to address new and emerging needs, challenges, and issues13–15 and increase citizen engagement and community ownership of health services. In Ghana, use of scorecards to engage multiple stakeholders to improve maternal health services resulted in improved care, in addition to an improved culture of accountability, increased community participation and transparency, and clarified lines of accountability among decision makers.16 Evaluation of a maternal health citizen monitoring process in Peru’s Puno region, found it contributed to greater respect and cultural sensitivity in service delivery, staff becoming more responsive to users’ needs, and increased use of services, among other outcomes.17
Poor policy implementation and budget allocation to health facilities lead to poor services, inequities, and discrimination. Social accountability processes have led to better defined and coordinated policies, budgets, and plans including increased ability of providers and managers to advocate for needs with higher levels of the health system (e.g., state/province or national), and increased allocation and reallocation of resources,18–25 including for marginalized groups. Social accountability processes facilitate this by strengthening health facility committees, which are often the interface between communities and facilities,26,27 enabling health providers to better understand the needs of the communities they serve. Further, aligning services with needs can produce a good return on investment: experience in Nigeria showed that investing in a social accountability process could results in a cumulative social return on investment of 13 Naira for every 1 Naira invested in the next five years.28
Lack of trust in the health system discourages people from accessing services. The process of sharing information, discussion, and negotiation can transform trust within health systems. In India, social accountability processes improved trust and collaboration between women and the health system, in turn increasing use of maternal health services.29** Use of community scorecards in humanitarian settings, has been shown to build trust and increase service utilization.30 In Sierra Leone, areas involved in social accountability processes two years prior to the Ebola outbreak in 2014–2015 had higher reporting of Ebola cases as well as lower mortality from Ebola.31
When communities are unaware of their rights and entitlements, or have low self-efficacy to obtain them, they are less likely to demand them from health sector actors. Accountability is a cornerstone of ensuring that human rights, including the right to the highest attainable standard of sexual and reproductive health, are upheld. Social accountability has promoted greater awareness of rights among citizens and health sector actors.18,20,22,23,32 In Uganda, a social accountability initiative resulted in increased awareness of health issues, knowledge about entitlements and expected standards of care, confidence in the health system, and empowerment to raise voices.32 In Bangladesh, ”NariDal” groups have brought together women, including those from marginalized communities, to monitor and discuss the provision of high-quality health care services, resulting in increased awareness of health rights, use of the health services, and accountability in service provision.33
Social determinants, specifically unequal power dynamics and gender norms, create barriers to family planning use. Social accountability efforts can confront and transform adverse power relationships34–36 by providing space for different groups (e.g., women, men, youth, local leaders, and providers, including the most vulnerable in communities) to share issues and to make sure their voices are heard and not drowned out by the more powerful.15,23,37 Additionally, social accountability efforts can address imbalances in access to information. As health sector actors gain awareness of community needs and priorities, their attitudes towards citizens and communities can also improve, along with stronger community/service provider relationships and greater legitimacy, credibility, and trust.
**Trust was described qualitatively as: feeling welcomed by facility staff; perceived equal and fair treatment; understanding and ease in interactions with health facility staff.
What is the impact?
Social accountability mechanisms support the development of an enabling environment for family planning programs. Specifically, social accountability programs can disrupt and realign the governance structures and systems that affect an individual’s ability to access family planning information and services. The evidence base on social accountability in reproductive health is growing.21,30,38–42 Several reviews of social accountability interventions in reproductive health have concluded that these approaches can lead to localized improvements in service delivery and client-provider relationships.7,14,18,21,43 The strongest evidence related to the intermediate and HIPs outcomes is from Malawi and Uganda (Table 1), with more evidence forthcoming from Ghana and Tanzania.44,45
Social accountability interventions have made family planning services more responsive to client needs. Across social accountability interventions, providers and clients have reported improvements in services. In a study in Malawi, communities and providers identified issues to address, agreed on indicators of progress, and met every six months to measure these through CSC. There were improvements in the 13 indicators on the scorecard over a two-year period, with 10 of the improvements being statistically significant (Figure 2).19 For example, communities and providers observed statistically significant improvements in the relationship between clients and providers, the way clients were greeted, health worker commitment, level of male engagement and youth involvement, and availability and accessibility of information.
Since social accountability is intended to improve client experience, system responsiveness, and equitable access, among other factors, evidence of the direct effects on contraceptive use and continuation is more limited. A social accountability intervention in Uganda resulted in a 60% statistically significant increase in the number of clients seeking family planning.46 Similarly, analysis of a CSC approach in Malawi found a non-significant increase in family planning use between the intervention and control group from baseline to endline. Further analysis suggests the CSC could have had a significant effect on the use of modern contraception, with a projected 57% greater use of family planning in the intervention versus control condition at endline.19 Forthcoming studies from Tanzania and Ghana should provide additional information on contraceptive use dynamics related to social accountability processes.44,45
Statistically significant positive effects of social accountability initiatives that included family planning and intervention/control groups on HIPs outcomes and intermediate outcomes from the theory of change
| Country and reference | Intervention | Intermediate outcomes/benefits | HIPs outcomes (reported by providers) | HIPs outcomes (reported by clients/communities) |
|---|---|---|---|---|
| Malawi
Gullo et al., 201719; Gullo et al., 201837; Gullo et al., 202048 |
CARE Community Score Card (CSC) using cyclical process, every six months over two years with community members (men, women, youth, vulnerable groups, power holders), health providers, and power holders (including District Health Management Team): (1) meetings (community and providers separately) to identify barriers/facilitators to service use and delivery, and develop measurable indicators (i.e., scorecard); (2) interface meetings to develop plans; and (3) action plan implementation and monitoring. | From Gullo et al., 201837:
Community members have increased ability to express needs and participate in dialogue with health actors*
Solutions are implemented and collectively monitored, with adaptations as needed
|
From Gullo et al., 202048:
Health resources and services more equitably distributed, leading to improved access and use among vulnerable populations
Health sector actors’ capacity to deliver quality and equitable family planning care is strengthened
|
From Gullo et al., 201719:
Client experienced improved quality of care that is responsive to their needs
|
| Uganda
Björkman & Svensson, 200946; Donato et al., 201948 |
Community report card approach with community member meetings to discuss report card and rights, and to develop and prioritize a plan to improve services; a meeting with the health facility to discuss report card; an interface meeting to discuss and develop a shared action plan (including monitoring), and follow-up meetings over six months. Replication. Donato et al., 201948 used data from Björkman & Svensson (2009)46 to replicate and extend analyses (e.g., include process measures, assess and address balance in treatment and comparison communities). Analyses yielded similar results in terms of health care provider behaviors and client service utilization. |
Community members have increased ability to express needs and participate in dialogue with health actors
|
Improved quality of care provision that is responsive to client needs
Health sector actors’ capacity to deliver quality and equitable family planning care is strengthened
|
Clients experience improved quality of care that is responsive to their needs
|
*Among 284 women in intervention communities aware of CSC (around one quarter of the sample in the treatment area), assessed association between participation (yes/no) and intermediate governance outcomes.
Change in Community Score Card from first to final measure19

How to do it: Tips from implementation experience
Set the stage for a collaborative process. Securing buy-in and meaningful participation of health system actors is key to success.49 Practitioners have found the following processes helpful in overcoming initial resistance from key government stakeholders who may feel uncomfortable:
- Provide space at the beginning of the process to sensitize different actors on health rights, family planning, responsibilities, and accountability. This can help ensure everyone has investment in the process, the challenges of different actors (community and health facility staff) are understood, misconceptions are addressed, and there is mutual understanding and respect.32
- Health officials and service providers may fear being attacked and blamed; giving them an opportunity to express their frustrations and vocalize those feelings, as well as assuring them that the process is not about finger-pointing and blame is an important first step. For example, orientation meetings with service providers can include providers anonymously submitting concerns/fears on paper so they can be addressed and discussed.50
- Prior to meeting with the frontline health workers, sessions with district-level health officials and managers can focus on how the approach can help solve issues they face (e.g., targeting limited resources, improving health indicators), clarify roles and responsibilities,16 and facilitate shared ownership of the process. It can be helpful to have health officials who have gone through the process share their experiences with their peers, describing how it works and the benefits. In some cases, adapting language can help smooth the way, i.e., focusing on improvements in quality, equity, and responsiveness, as opposed to stressing “rights” and “accountability” as key phrases.
- Take the time to listen to health providers and analyze with them what the barriers are to providing responsive services, what they would like to see change, and what benefits might come from participation in the process. This can go a long way toward building trust and meaningful participation.
- Finally, securing buy-in and engagement from community members and health facility staff is a continuous process; lack of participation and motivation will limit the effectiveness of social accountability approaches.2
Identify the right problems to address. Every community and context is different, and not all problems can be addressed through a collaborative social accountability process.
- It is important to understand the context when selecting a social accountability approach and tools; tools and approaches used in “one setting may not achieve the same outcomes in a different setting.”51(p3) Collaborative approaches require participation and buy-in from health system actors, which may not be a realistic expectation in some contexts.
- Working with the community and health system stakeholders to identify and respond to needs they themselves identify is crucial. Further, it is important that interventions are informed by and developed with a diverse range of locally relevant stakeholders from the community and the health facility/system, so that they are tailored to their needs and contexts.
- Be mindful of, and adapt to, the contextual factors that may limit participation by community members, including literacy, social determinants (the conditions in which people are born, work, and live), gender norms, and power dynamics and trust within the community and between the community and the health facility/system.8,23,35,52–54
A structured and facilitated process built on transparency, inclusion, equity. Social accountability processes should be built on raising awareness among health providers and communities about their rights and entitlements, and standards of client-centered family planning care they should receive, as well as information about the quality and characteristics of services currently available to them. Furthermore, understanding of social/gender/cultural norms and ensuring opinion leaders are fully involved is critical to undertaking social accountability processes.
Promote dialogue, negotiation, and collective action. Ensuring a supportive environment where everyone—from marginalized groups to health workers—feel listened to, understood, and not blamed or reproached, can lead to improved service delivery and policy outcomes.51 This safe space can be facilitated through the following processes:
- Ensure good and practiced facilitation, which recognizes and seeks to alter the existing power imbalances within the community and between the community and health facility/system.29
- Combine activities: combining health education, outreach, civic education, and community dialogue can be beneficial in addressing local gender dynamics, which can affect women and young people’s ability to participate in community sensitization or outreach services.23
- Ensure communities direct how best their requests and demands are communicated, especially where they fear potential reprisal. Emphasis must be put on creating “safe spaces” that allow actors to express themselves and share information in ways that might be novel, challenging hierarchies and fostering more positive perceptions around family planning.32
- Conduct discussions with specific segments of the population (e.g., women, youth, persons with disabilities) to ensure that marginalized voices are not overpowered by those who are more dominant within the community.51
- Experienced, well-trained facilitators are essential to managing relationships, and ensuring regular and productive interactions between health facility staff and the community.18 Social accountability processes are often best facilitated by a neutral third party.
Sustainability. Effective social accountability approaches can contribute to the increased resilience of the health system even in times of crises.31 To be sustainable, communities need to value the social accountability approaches and see their continued utility in addressing their needs.19 This becomes particularly acute where domestic or international organizations have laid the groundwork for social accountability approaches, because they have the resources and person-power to facilitate the necessary relationships and help broker the power dynamics between community and facility that can stymie discussion and resolution. Involvement of community partners in social accountability efforts could include incentives to ensure continued participation.52
Box 2. Youth Adapt Community Score Card Approach to Address a Range of SRH and Other Issues15
A retrospective study in Malawi showed youth adapted the Community Score Card approach to address other issues of importance to them, including SRH, child marriage, girls’ education, and natural resources and protection of the environment. In a follow-up study, some young people mentioned increased contraceptive use and decreasing unintended pregnancies among youth, as outcomes from the continued use of the CSC. They also mentioned that young people who participated in the CSC believed they do not have to wait for others to address issues of importance to them; instead, they are empowered to have a role in the governance of their community. They recommended nationwide scale-up of the CSC.
Implementation measurement
Measuring social accountability is challenging given its complexity.55,56 Building on measures developed in Malawi,18 the CaPSAI study has tested and validated measures that can be used to explore a range of social accountability outcomes.57 The following indicators may be helpful in measuring implementation and outcomes:
- Percent of community/health facility catchment areas that have functional mechanisms for engaging communities (especially women and marginalized groups) in the design, implementation, and monitoring of family planning service delivery
- Percent of women and/or number of marginalized groups who participate in functional accountability mechanisms that include family planning
- Clients in the catchment area with social accountability mechanisms experience improved quality of care that is respectful and responsive to their family planning needs (e.g., measured from community scorecards)
Priority Research Questions
Social accountability is a complex intervention with a need for mixed methods studies. Key research priorities include:
- What factors promote the integration, scalability, and sustainability of social accountability processes geared to improving the quality and utilization of family planning services?16,22,51
- How, if at all, can accountability at global, regional, and national levels be aligned with local social accountability initiatives (e.g., community scorecards) for system-wide change in family planning?51,58
- How can social accountability approaches designed to improve family planning outcomes work in settings where there is less community cohesion and less spare time to participate in community activities, e.g., urban areas, countries responding to shocks (e.g., armed conflict, climate- and pandemic-related conflict), pastoralist communities, and areas with internally displaced persons?
- How can we best measure increases in trust as an outcome of social accountability initiatives?
Tools and Resources
- Social Accountability Resources and Tools. Intended to assist civil society organizations, non-governmental organizations, and government health program planners, managers, and staff to identify and adapt existing guides and tools for effective social accountability strategies.
- Citizen Voice & Action Field Guide. A guide to a local-level advocacy methodology that transforms the dialogue between communities and government in order to improve services that affect the lives of children and their families.
- CARE’s Community Score Card© (CSC) is a citizen-driven accountability approach for the assessment, planning, monitoring, and evaluation of public services. It enables community members, health providers, and government officials to work together to identify and overcome health coverage quality and equity obstacles.
- Community Score Card Implementation Guidance Note. Recommendations for CARE CSC Experts.
- Accountability Measurement Framework Tool. Has been used across the Women’s Integrated Sexual Health programme to help explore if and how accountability initiatives are functioning effectively and contributing to improving family planning outcomes in their contexts.59
References
- Houtzager P, Joshi A. Introduction: contours of a research project and early findings. IDS Bulletin. 2008;38(6):1–9. Accessed May 17, 2022. https://core.ac.uk/download/pdf/286043915.pdf
- Danhoundo G, Nasiri K, Wiktorowicz ME. Improving social accountability processes in the health sector in sub-Saharan Africa: a systematic review. BMC Public Health. 2018;18(1):497. https://doi.org/10.1186/s12889-018-5407-8
- McGinn E, Lipsky A. Social Accountability: A Primer for Civil Society Organizations Working in Family Planning and Reproductive Health. Health Policy Project; 2015. Accessed May 17, 2022. https://www.healthpolicyproject.com/pubs/449_PSocialAccountabilityReportFINALEC.pdf
- Sirker K, Cosic S; Public Affairs Foundation. Empowering the Marginalized: Case Studies of Social Accountability Initiatives in Asia. WBI Working Papers. World Bank Institute; 2007. Accessed May 17, 2022. https://www.researchgate.net/publication/240641681_Empowering_the_Marginalized_Case_Studies_of_Social_Accountability_Initiatives_in_Asia
- Joshi A. Do they work? Assessing the impact of transparency and accountability initiatives in service delivery. Dev Policy Rev. 2013;31(S1):S29–S48. https://doi.org/10.1111/dpr.12018
- Fox JA. Social accountability: what does the evidence really say? World Dev. 2015;72:346–361. https://doi.org/10.1016/j.worlddev.2015.03.011
- [impact] Waddington H, Sonnenfeld A, Finetti J, Gaarder M, John D, Stevenson J. Citizen engagement in public services in low- and middle-income countries: a mixed-methods systematic review of participation, inclusion, transparency and accountability (PITA) initiatives. Campbell Syst Rev. 2019;15(1–2):e1025. https://doi.org/10.1002/cl2.1025
- Squires F, Martin Hilber A, Cordero JP, et al. Social accountability for reproductive, maternal, newborn, child and adolescent health: a review of reviews. PLoS One. 2020;15(10):e0238776. https://doi.org/10.1371/journal.pone.0238776
- Boydell V, Keesbury J. Social Accountability: What Are the Lessons for Improving Family Planning and Reproductive Health Programs? A Review of the Literature. Working Paper. Population Council, Evidence Project; 2014. Accessed May 17, 2022. https://knowledgecommons.popcouncil.org/cgi/viewcontent.cgi?article=1942&context=departments_sbsr-rh
- Sneeringer RK, Hurd SE, Mehling KC, Motihar R, Akpan T, Rukundo D. Engendering Accountability: Upholding Commitments to Maternal and Newborn Health. Global Health Visions; 2015. Accessed May 17, 2022. https://uploads-ssl.webflow.com/5a25e6430f93020001836dfa/5e248ead2e290c32b9d26ce0_EngenderingAccountabilityReport.pdf
- Katende S. Citizen Voice and Action (CVA) Model. Field Practitioner Version. Evidence 4 Change. World Vision Middle East and Eastern Europe Regional Office; 2018. Accessed May 17, 2022. https://www.wvi.org/sites/default/files/CVA%20with%20proofreading%20final.pdf
- Ralidera, OR. Removing Taxes for Contraceptives in Madagascar: Strategic Advocacy Leads to Increased Budget for Family Planning. IBP Network; 2021. Accessed May 17, 2022. https://d1c2gz5q23tkk0.cloudfront.net/assets/uploads/3082408/asset/Options_Madagascar.pdf
- Björkman Nyqvist M, de Walque D, Svensson J. Information Is Power: Experimental Evidence on the Long-Run Impact of Community Based Monitoring. Policy Research Working Paper 7015. World Bank; 2014. Accessed May 17, 2022. https://openknowledge.worldbank.org/bitstream/handle/10986/20364/WPS7015.pdf
- [impact] CARE. Government-led Community Score Card© for Family Planning Services. CARE; 2020. Accessed May 17, 2022. https://insights.careinternational.org.uk/media/k2/attachments/CARE_Government-led-CSC-family-planning-services_July-2020.pdf
- Mgoli Mwale P, Msiska T, Wako E, et al. Evaluating young people’s ability to sustain an evidence-based social accountability approach to improve adolescent sexual and reproductive health in Ntcheu, Malawi. Front Reproductive Health. 2021;3:645280. https://doi.org/10.3389/frph.2021.645280
- Blake C, Annorbah-Sarpei NA, Bailey C, et al. Scorecards and social accountability for improved maternal and newborn health services: A pilot in the Ashanti and Volta regions of Ghana. Int J Gynaecol Obstet. 2016;135(3):372–379. https://doi.org/10.1016/j.ijgo.2016.10.004
- CARE. Citizen Monitoring to Defend Maternal Health Rights in Peru. Learning and Policy Series Issue 6. CARE; 2015. Accessed May 17, 2022. https://insights.careinternational.org.uk/media/k2/attachments/CARE_Citizen-monitoring-in-Peru_2015.pdf
- [impact] Gullo S, Galavotti C, Altman L. A review of CARE’s Community Score Card experience and evidence. Health Policy Plan. 2016;31(10):1467–1478. https://doi.org/10.1093/heapol/czw064
- [impact] Gullo S, Galavotti C, Sebert Kuhlmann A, Msiska T, Hastings P, Marti CN. Effects of a social accountability approach, CARE’s Community Score Card, on reproductive health-related outcomes in Malawi: a cluster-randomized controlled evaluation. PLoS One. 2017;12(2):e0171316. https://doi.org/10.1371/journal.pone.0171316
- Ball D, Westhorp G. Citizen Voice and Action for Government Accountability and Improved Services: Maternal, Newborn, Infant and Child Health Services. Final Evaluation Report. Community Matters Pty Ltd.; 2018. Accessed May 17, 2022. https://documents1.worldbank.org/curated/en/331651607355519716/pdf/Final-Evaluation-Report.pdf
- [impact] Wild L, Wales J, Chambers V. CARE’s Experience With Community Score Cards: What Works and Why? Synthesis Report. ODI; 2015. Accessed May 17, 2022. https://cdn.odi.org/media/documents/9451.pdf
- Schaaf M, Topp SM, Ngulube M. From favours to entitlements: community voice and action and health service quality in Zambia. Health Policy Plan. 2017;32(6):847–859. https://doi.org/10.1093/heapol/czx024
- Boydell V, Neema S, Wright K, Hardee K. Closing the gap between people and programs: lessons from implementation of social accountability for family planning and reproductive health in Uganda. Afr J Reprod Health. 2018;22(1):73–84. https://doi.org/10.29063/ajrh2018/v22i1.7
- Women’s Integrated Sexual Health (WISH2Action). Ensuring the Continuity of Government Sexual and Reproductive Health/Family Planning Services During the COVID-19 Pandemic: Experiences and Lessons From the Women’s Integrated Sexual Health (WISH2Action) Programme. WISH2Action Learning Brief. WISH2Action; 2020. https://options.co.uk/sites/default/files/ensuring_the_continuity_of_government_sexual_andreproductive_health_and_family_planning_services_during_the_covid-19_pandemic_0.pdf
- E4A-MamaYe. Impact Report 2018-2019. Options Consultancy Services; 2019. Accessed May 17, 2022. https://mamaye.org/sites/default/files/docs/IMPACT_Report20182019.pdf
- Grellier R. Grants to community groups lead to positive change in healthcare. Options. December 4, 2018. Accessed May 17, 2022. https://options.co.uk/news/grants-to-community-groups-lead-to-positive-change-in-healthcare
- Lodenstein E, Molenaar JM, Ingemann C, et al. “We come as friends”: approaches to social accountability by health committees in Northern Malawi. BMC Health Serv Res. 2019;19(1):279. https://doi.org/10.1186/s12913-019-4069-2
- Maternal, Newborn and Child Health Programme (MNCH2). Measuring the Benefits to the Communities They Serve: The Social Return on Investment of Community Accountability Mechanisms for Health. MNCH2; 2019. Accessed May 17, 2022. https://options.co.uk/sites/default/files/community_accountability_mechanisms_for_health_measuring_the_benefits_to_the_communities_they_serve.pdf
- Hamal M, de Cock Buning T, De Brouwere V, Bardají A, Dieleman M. How does social accountability contribute to better maternal health outcomes? A qualitative study on perceived changes with government and civil society actors in Gujarat, India. BMC Health Serv Res. 2018;18(1):653. https://doi.org/10.1186/s12913-018-3453-7
- [impact] Ho LS, Labrecque G, Batonon I, Salsi V, Ratnayake R. Effects of a community scorecard on improving the local health system in Eastern Democratic Republic of Congo: qualitative evidence using the most significant change technique. Confl Health. 2015;9:27. http://dx.doi.org/10.1186/s13031-015-0055-4
- Christensen D, Dube O, Haushofer J, Siddiqi B, Voors M. Building Resilient Health Systems: Experimental Evidence From Sierra Leone and the 2014 Ebola Outbreak. Working Paper 526. Center for Global Development; 2020. Accessed May 17, 2022. https://www.cgdev.org/sites/default/files/building-resilient-health-systems-experimental-evidence-sierra-leone-and-2014-ebola.pdf
- Boydell V, Nulu N, Hardee K, Gay J. Implementing social accountability for contraceptive services: lessons from Uganda. BMC Womens Health. 2020;20(1):228. https://doi.org/10.1186/s12905-020-01072-9
- Afrin S, Barpanda S, Das A. Women in the Lead: Monitoring Health Services in Bangladesh. COPASAH Series on Social Accountability, Case Study 1. Centre for Health and Social Justice; 2015. Accessed May 17, 2022. http://www.chsj.org/uploads/1/0/2/1/10215849/case_study_1.pdf
- Sen G, Iyer A, Chattopadhyay S, Khosla R. When accountability meets power: realizing sexual and reproductive health and rights. Int J Equity Health. 2020;19(1):111. https://doi.org/10.1186/s12939-020-01221-4
- Niyongabo P, Douwes R, Dieleman M, et al. Ways and channels for voice regarding perceptions of maternal health care services within the communities of the Makamba and Kayanza provinces in the Republic of Burundi: an exploratory study. BMC Health Serv Res. 2018;18(1):46. https://doi.org/10.1186/s12913-017-2822-y
- Boydell V, Schaaf M, George A, Brinkerhoff DW, Van Belle S, Khosla R. Building a transformative agenda for accountability in SRHR: lessons learned from SRHR and accountability literatures. Sex Reprod Health Matters. 2019;27(2):1622357. https://doi.org/10.1080/26410397.2019.1622357
- Gullo S, Kuhlmann AS, Galavotti C, Msiska T, Nathan Marti C, Hastings P. Creating spaces for dialogue: a cluster-randomized evaluation of CARE’s Community Score Card on health governance outcomes. BMC Health Serv Res. 2018;18(1):858. https://doi.org/10.1186/s12913-018-3651-3
- [impact] Martin Hilber A, Blake C, Bohle LF, Bandali S, Agbon E, Hulton L. 2016. Strengthening accountability for improved maternal and newborn health: a mapping of studies in sub-Saharan Africa. Int J Gynaecol Obstet. 2016;135(3):345–357. https://doi.org/10.1016/j.ijgo.2016.09.008
- [impact] Lodenstein E, Dieleman M, Gerretsen B, Broerse JE. Health provider responsiveness to social accountability initiatives in low- and middle-income countries: a realist review. Health Policy Plan. 2017;32(1):125–140. https://doi.org/10.1093/heapol/czw089
- [impact] Mohanan M, Thirumurthy H, Rajan V. Mobilizing Communities for a Healthier Future: Impact Evaluation of Social Accountability Interventions in Uttar Pradesh, India. World Bank; 2018. Accessed May 17, 2022. https://documents1.worldbank.org/curated/en/340831537776397782/pdf/UP-SA-Final-Report.pdf
- [impact] Van Belle S, Boydell V, George AS, Brinkerhoff DW, Khosla R. Broadening understanding of accountability ecosystems in sexual and reproductive health and rights: a systematic review [published correction appears in PLoS One. 2018 Jul 10;13(7):e0200675]. PLoS One. 2018;13(5):e0196788. https://doi.org/10.1371/journal.pone.0196788
- [impact] Edward A, Jung Y, Chhorvann C, Ghee AE, Chege J. Can social accountability mechanisms using community scorecards improve quality of pediatric care in rural Cambodia?. Int J Qual Health Care. 2020;32(6):364–372. https://doi.org/10.1093/intqhc/mzaa052
- [impact] Holland J, Schatz F, Befani B, Hughes C. Macro Evaluation of DFID’s Policy Frame for Empowerment and Accountability Empowerment and Accountability. Empowerment and Accountability Annual Technical Report 2016: What Works for Social Accountability. Final Version. e-Pact Consortium; 2016. Accessed May 17, 2022. https://itad.com/wp-content/uploads/2017/06/EA-Macro-Evaluation-Technical-report-Dec16-FINAL.pdf
- [impact] Steyn PS, Boydell V, Cordero JP, et al. Rationale and design of a complex intervention measuring the impact and processes of social accountability applied to contraceptive programming: CaPSAI Project. Gates Open Res. 2020;4:26. https://doi.org/10.12688/gatesopenres.13075.2
- [impact] McMullen H, Boydell V, Cordero JP, et al. Accounting for complexity – Intervention design in the context of studying social accountability for reproductive health [version 1; peer review: 3 approved with reservations]. Gates Open Res. 2021;5:107. https://doi.org/10.12688/gatesopenres.13260.1
- [impact] Björkman M, Svensson J. Power to the people: evidence from a randomized field experiment on community-based monitoring in Uganda. Q J Econ. 2009;124(2):735–769. https://doi.org/10.1596/1813-9450-4268
- Gullo S, Galavotti C, Sebert Kuhlmann A, Msiska T, Hastings P, Marti CN. Effects of the Community Score Card approach on reproductive health service-related outcomes in Malawi. PLoS One. 2020;15(5):e0232868. https://doi.org/10.1371/journal.pone.0232868
- Donato K, Garcia Mosqueira A. Information improves provider behaviour: a replication study of a community-based monitoring programme in Uganda. J Dev Stud. 2019;55(5):967–988. https://doi.org/10.1080/00220388.2018.1506577
- World Health Organization (WHO). Community and Provider-Driven Social Accountability Intervention for Family Planning and Contraceptive Service Provision: Experiences From the Field. WHO; 2021. Accessed May 17, 2022. https://apps.who.int/iris/handle/10665/350839
- CARE Malawi. The Community Score Card (CSC): A Generic Guide for Implementing CARE’s CSC Process to Improve Quality of Services. CARE; 2013. Accessed May 18, 2022. https://www.care.org/wp-content/uploads/2020/05/FP-2013-CARE_CommunityScoreCardToolkit.pdf
- Hurd S, Folse M, Fox S. In Brief: Evidence on the Role of Social Accountability in Advancing Women, Children, and Adolescents’ Health. Global Health Visions; 2020. Accessed May 17, 2022. https://uploads-ssl.webflow.com/5a25e6430f93020001836dfa/5f31f7829eff9b132b7342b3_Social%20Accountability%20Brief_0720.pdf
- Solnes Miltenburg A, van Pelt S, de Bruin W, Shields-Zeeman L. Mobilizing community action to improve maternal health in a rural district in Tanzania: lessons learned from two years of community group activities. Glob Health Action. 2019;12(1):1621590. https://doi.org/10.1080/16549716.2019.1621590
- Brinkerhoff DW, Wetterberg, A. Gauging the effects of social accountability on services, governance, and citizen empowerment. Public Adm Rev. 2015;76(2):274–286. https://doi.org/10.1111/puar.12399
- Ogbuabor DC, Onwujekwe OE. The community is just a small circle: citizen participation in the free maternal and child healthcare programme of Enugu State, Nigeria. Glob Health Action. 2018;11(1):1421002. https://doi.org/10.1080/16549716.2017.1421002
- Boydell V, McMullen H, Cordero J, Steyn P, Kiare J. Studying social accountability in the context of health system strengthening: innovations and considerations for future work. Health Res Policy Syst. 2019;17(1):34. https://doi.org/10.1186/s12961-019-0438-x
- Schaaf M, Cant S, Cordero J, Contractor S, Wako E, Marston C. Unpacking power dynamics in research and evaluation on social accountability for sexual and reproductive health and rights. Int J Equity Health. 2021;20(1):56. https://doi.org/10.1186/s12939-021-01398-2
- Boydell V, Steyn PS, Cordero JP, et al. Adaptation and validation of social accountability measures in the context of contraceptive services in Ghana and Tanzania. Int J Equity Health. 2020;19(1):183. https://doi.org/10.1186/s12939-020-01286-1
- Fox J. How can a rethink of lessons from field experiments inform future research in transparency, participation and accountability? Evidence Matters blog. May 29, 2019. Accessed May 17, 2022. https://www.3ieimpact.org/blogs/how-can-rethink-lessons-field-experiments-inform-future-research-transparency-participation
- Martin Hilber A, Doherty P, Nove A, Cullen R, Segun T, Bandali S. The development of a new accountability measurement framework and tool for global health initiatives. Health Policy Plan. 2020;35(7):765–774. https://doi.org/10.1093/heapol/czz170
Suggested Citation
High Impact Practices in Family Planning (HIPs). Social accountability to improve family planning information and services. Washington, DC: HIPs Partnership; August 2022. Available from: https://fphighimpactpractices.org/briefs/social-accountability/
Acknowledgements
This brief was written by: Victoria Boydell (Geneva Graduate Institute), Patricia ‘Trish’ Doherty (Options Consultancy Services Limited), Jeanne Fournier (Equipop), Christine Galavotti (BMGF), Carolyn Grant (CARE), Sara Gullo, Karen Hardee (What Works Association), Kamden Hoffman (CORUS International), Joan Kraft (USAID), Shawn Malarcher (USAID), Tanvi Monga (Margaret A. Cargill Philanthropies), and Petrus Steyn (WHO).
This brief was reviewed and approved by the HIPs Technical Advisory Group. In addition, the following individuals and organizations provided critical review and helpful comments: Maria Carrasco (USAID), Carolyn Grant (CARE), Alyson Lipsky (RTI International), and Martha Murdock (MSH).
The World Health Organization/Department of Sexual and Reproductive Health and Research has contributed to the development of the technical content of HIPs briefs, which are viewed as summaries of evidence and field experience. It is intended that these briefs be used in conjunction with WHO Family Planning Tools and Guidelines: https://who.int/health-topics/contraception
The HIPs Partnership is a diverse and results-oriented partnership encompassing a wide range of stakeholders and experts. As such, the information in HIPs materials does not necessarily reflect the views of each co-sponsor or partner organization.
To engage with the HIPs please go to: https://fphighimpactpractices.org/engage-with-the-hips/